01 — The Problem
A transition built for charts, not for teenagers.
Adolescents with chronic illnesses face a double burden when leaving pediatric care: their medical plans are technically sound, but built for a world that doesn't account for social reality. The result is missed doses, unnecessary ER visits, and a collapse in self-management confidence at exactly the moment it matters most.
"A young patient with a chronic illness who feels anxious about managing their own care needs to transition into the adult healthcare system independently, but social stigma, lack of peer support, and dependence on caregivers create barriers."
+40%
Adherence
In patients who view care as part of their identity
73%
Behavioral Shift
Of AYA modify routines to avoid public stigma
-27%
Adherence Drop
In the afternoon due to decision fatigue
+60%
ER Visits
In the first year after abrupt transition from pediatric care
02 — Research & Findings
What the interviews revealed.
We structured primary research across four inquiry areas to understand the full landscape of the adolescent healthcare transition: daily management logistics, information-seeking behavior, emotional experience, and caregiver dynamics.
Routine Reliance
Management depends on multiple daily alarms and physical medication bags, creating a visible and stigma-prone routine.
Caregiver Dependency
Mothers remain deeply involved as "back-up" systems for alarms and school logistics, making the handoff to independence harder.
Stigma & Privacy
Fear of being stared at while taking medication in public leads to missed doses and dangerous treatment delays.
Identity Shift
The transition isn't just logistical — it requires becoming an adult who owns their health, not just a "kid patient."
Peer Connection
AYA place high value on near-peer mentorship. Hearing from someone "like me" is as vital as clinical education.
Perspective Gap
Clinicians may rate a condition as "mild" while the teen experiences it as life-defining due to daily stigma and logistical burden.
03 — Strategic Insights
Five principles that shaped the design.
Identity Over Compliance
Build tools that make teens feel like independent adults, not patients.
Reduce, Don't Remind
Use "chunking" to minimize active decision-making and cognitive load.
Invisible Design
Tools should look like fashion or tech accessories, not medical gear.
Supported Autonomy
"Break-Glass" caregiver access: watch from a distance, intervene only in crisis.
The Near-Peer Bridge
AYA trust doctors for labs — but they trust peers for life.
04 — The Solution
MAYA: Mentor for Adolescents and Young Adults.
MAYA is an identity-focused mobile ecosystem that moves beyond clinical tracking to support the person, not just the patient. It looks and feels like a modern wellness companion — something a teen is proud to use in front of friends, not hide.
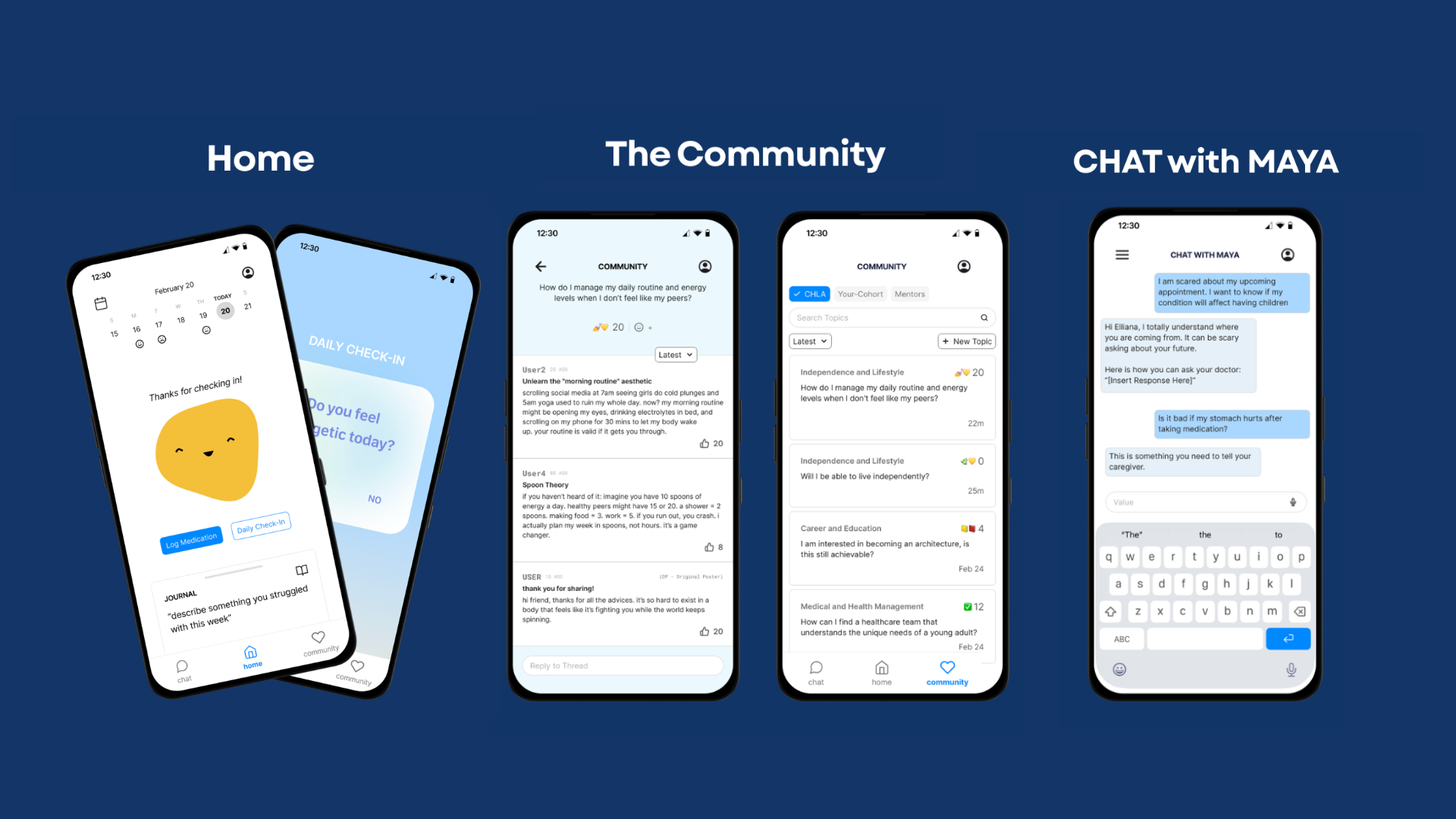
Home Dashboard
Track & Reflect
Mood, medication & symptom logging; animated MAYA companion; journal with free-write prompts
Chat with MAYA
Ask & Practice
AI-powered Q&A; appointment "practice mode"; never prescribes — always defers to providers
Community
Connect & Learn
Peer-reviewed forum; near-peer mentor matching; vetted influencers who have completed transition
01
No Prescriptions
MAYA never prescribes treatment — it helps teens formulate questions for their real providers.
02
Emotional Mirroring
The animated "blob" mascot shifts expression with the user's check-in, providing empathy without clinical surveillance.
03
Break-Glass Access
Caregiver visibility is passive by default, with active involvement only in crisis situations.
05 — Next Steps
Where MAYA goes from here.
01
Backstory Thread
A portable patient history that helps new adult providers understand context and trust triggers instantly.
02
Caregiver Dashboard
Reduce active monitoring milestones over time, moving caregiver oversight to a crisis-only model.
03
Knowledge Base
Continuously update with clinician-approved content focused on the social and emotional realities of emerging adulthood.
Reflection
Designing for identity, not just illness.
This project pushed me to think beyond feature design toward the emotional and identity work that underpins behavior change. One of the biggest takeaways was that what appears "mild" in clinical documentation can be life-defining in a teenager's day-to-day experience.
Conversations with staff and young adults who had already gone through this process revealed that many adolescents aren't lacking awareness — they often just need the support and encouragement to begin asking questions themselves and gradually step into conversations independently.
Working directly with CHLA grounded the research in real institutional constraints, from peer mentor moderation to clinician approval workflows, forcing our team to think beyond ideal solutions and propose systems that could realistically operate within healthcare environments.